Bacterial Vaginosis (BV)
Overview
What is BV?
BV is a mild infection of the vagina caused by an imbalance in the growth of the bacteria that normally populate the vagina – it is not known exactly why this imbalance in bacterial growth occurs. This condition used to be called Gardnerella vaginitis, because Gardnerella is a type of bacteria that sometimes causes the infection. We now know that overgrowth of other types of bacteria can also cause BV.
- Lactobacillus spp. is the most frequently isolated genus of bacteria found in the healthy vaginal flora – they play a role in maintaining the balance of the normal vaginal flora by producing hydrogen peroxide.
Unlike sexually transmitted infections:
- Infection results from bacteria that are normally found in the vagin a
- A woman does not get the infection from a sex partner – It is most common in sexually active women, but women who are not sexually active also can develop the condition.
BV can cause serious problems in pregnancy
Problems caused by BV. Screening for bacterial vaginosis and treatment if necessary during pregnancy can help prevent these complications.
- Premature labor / birth
- Infection of the amniotic fluid and uterus after delivery.
BV Medical Diagnosis
It is important to first exclude other serious infections – since vaginal discharge is also a symptom of other more dangerous infections, such as gonorrhea and chlamydia.
Medical diagnosis tests and criteria for BV
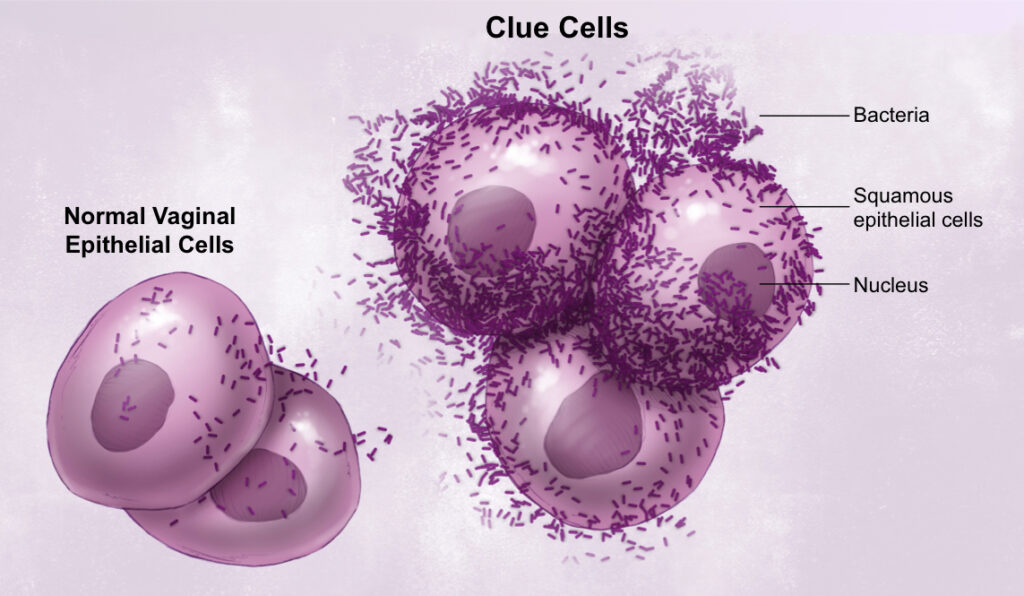
- Examining the vaginal discharge under the microscope can help distinguish bacterial vaginosis – from yeast vaginitis (candidiasis) and trichomonas (a type of sexually transmitted infection) – a sign of bacterial vaginosis under the microscope is an unusual vaginal cell called a clue cell. Clue cells are believed to be the most reliable diagnostic sign of bacterial vaginosis. In addition to clue cells, women with bacterial vaginosis have fewer of the normal vaginal bacteria, called lactobacilli. A vaginal pH greater than 4.5 is also suggestive of bacterial vaginosis.
- Whiff Test – the doctor may perform a “whiff test” with potassium hydroxide (KOH) liquid. When a drop of KOH testing liquid used in the “whiff test” contacts a drop of the discharge from a woman with bacterial vaginosis, a certain fishy odor can result.
- The Hay/Ison criteria :
- Grade 1 (Normal): Lactobacillus morphotypes predominate.
- Grade 2 (Intermediate): Mixed flora with some Lactobacilli present, but Gardnerella or Mobiluncus morphotypes also present.
- Grade 3 (Bacterial Vaginosis): Predominantly Gardnerella and/or Mobiluncus morphotypes. Few or absent Lactobacilli. Hay et al., 1994
- The Amsel criteria: At least three of the four criteria should be present for a confirmed diagnosis
- Thin, white, yellow, homogeneous discharge
- Clue cells on microscopy
- pH of vaginal fluid >4.5
- Release of a fishy odor on adding alkali—10% potassium hydroxide (KOH) solution.
For more in-depth information, please read this Bacterial Vaginosis article.
Symptoms of bacterial vaginosis (BV)
Bacterial vaginosis is not dangerous, but it can cause disturbing symptoms
Symproms vary among particular types of vaginitis, with some overlap:
- Vaginal discharge and odor that usually has an unpleasant odor, although 50% to 75% of women with the condition experience no symptoms. Discharge is generally grayish-white but can be of any color or consistency.
- Normal discharge is common when estrogen levels are high. Normal vaginal discharge is commonly milky white or mucoid, odorless, and non-irritating.
- Slight bleeding often occurs when estrogen levels abruptly decrease
- Discharge due to vaginitis is accompanied by pruritus (itching), vaginal soreness / redness from inflammation, and sometimes dysuria(burning, painful urination) or mild bleeding. Itching may interfere with sleep. Painful intercourse may also occur.
- In atrophic vaginitis. Discharge is scant, dyspareunia is common, and vaginal tissue appears thin and dry. Atrophic vaginitis is an inflammation of the vagina (and outer urinary tract) due to the thinning / shrinking of the tissues and decreased lubrication -all commonly due to lack of estrogen, which happens naturally during perimenopause and more so in post-menopause
In women of reproductive age. Vaginitis is usually infectious. The most common types are bacterial vaginosis, candidal vaginitis and trichomonal vaginitis (which is sexually transmitted).
Normally in women of reproductive age:
- Lactobacilli are the predominant constituent of normal vaginal flora . Their colonization keeps vaginal pH in the normal acidic range (3.8 – 4.2), thereby preventing overgrowth of pathogenic bacteria.
- High estrogen levels maintain vaginal thickness, bolstering local defenses
- Factors that predispose to overgrowth of bacterial vaginal pathogens. May include the following:
- An alkaline vaginal pH due to menstrual blood, semen, or a decrease in lactobacilli
- Poor hygiene
- Frequent douching
In postmenopausal women :
- Usually, a marked decrease in estrogen causes vaginal thinning, increasing vulnerability to infection and inflammation. Some treatments (eg, oophorectomy, pelvic radiation, certain chemotherapy drugs) result in loss of estrogen. Decreased estrogen predisposes to atrophic vaginitis.
- Poor hygiene. Can lead to chronic vulvar inflammation due to chemical irritation from urine or feces or due to nonspecific infection. (E.g. in patients who are incontinent or bedridden)
- Bacterial vaginosis, candidal vaginitis, and trichomonal vaginitis are uncommon among postmenopausal women. May occur in those with risk factors.
In women of all ages :
- Conditions that predispose to vaginal or vulvar infection include :
- Fistulas between the intestine and genital tract – allow intestinal flora to seed the genital tract
- Pelvic radiation or tumors – which break down tissue and thus compromise normal host defenses
- Non-infectious vulvitis accounts for up to 30% of vulvovaginitis cases, possibly resulting from hypersensitivity or irritant reactions. To hygiene sprays or perfumes, menstrual pads, laundry soaps, bleaches, fabric softeners, fabric dyes, synthetic fibers, bathwater additives, toilet tissue, or, occasionally, spermicides, vaginal lubricants or creams, latex condoms, vaginal contraceptive rings, or diaphragms
BV treatment options
General Guidelines
Don’t create an environment in GI tract and vaginal tract conducive to non-beneficial bacteria. Lay off the sugar and carbs (which turn to sugar after metabolism) – you’re giving the bacterial “unfriendlies” and fungi a reproductive party.
While the infection itself is not considered dangerous – if not treated, the bacteria may spread up into the uterus or fallopian tubes and lead to a more serious infection.
After treatment, the condition generally resolves without complications. However, up to 15% of women have recurrent symptoms that need to be treated with a second course of treatment.
Mainstream medical antibiotics
Metronidazole (Flagyl) and clindamycin (Cleocin) are examples of antibiotics that are effective in treating BV. Unfortunately, antibiotics kill off all bacteria (good and bad), which then creates more problems E.g. Yeast infection, weakens immune system.
Most recommended DIY treatment (hydrogen peroxide, folate, probiotics)
Do all 3 of the following both morning and night for 5 days:
(1) Douche with hydrogen peroxide – to reduce overpopulating unwanted bacteria. Fill the douche bottle with ½ cup water + ½ cup 3% hydrogen peroxide. Sit in shower and insert as far as you can and douche. Keep your knees up – it’s easier to hold inside. Try to hold it in for 5-10 minutes
(2) Take folate supplement – 800 mcg
(3) Use Lactobacillus species probiotics (E.g. L.. acidophilus and L. Bifidus) – to repopulate both the intestines and the vaginal tract with the “good guys”.
- Take oral probiotic dose – Minimum 10 billion CFUs per dose. This can be: (a) A quality probiotic supplement Or (b) A quality, high-probiotic yogurt with no added sugar (E.g. Organic Stonyfield, plain yogurt has the necessary numbers and types of live cultures)
- Put probiotic bacteria in the vagina – either place a probiotic capsule or a quality, probiotic-containing yogurt-soaked tampon in the vagina. For some extra “oof” to the therapy, you can first use a turkey baster to insert some yogurt into the vagina before inserting the yogurt-soaked tampon, which should hold the extra yogurt in place.
Boric acid powder for BV (or yeast infection)
Works by reacidifying vagina and killing off problem fungus and/or bacteria.
- Fill size zero gel capsules – with <2% boric acid powder (you can find it most pharmacies, it’s not the kind to get rid of cockroaches)
- Insert filled capsules into vagina nightly – as you’re lying down to go to bed, insert two gel (some ladies use only one with success) caps into vagina for 3- 10 days (until symptoms are gone), Staying flat helps to keep the boric acid inside of you. When you get up the next morning, you’ll need to wash off ooze.
- Boric acid is also used whilst taking antibiotics to prevent a yeast infection