Chronic Obstructive Pulmonary Disease (COPD)
What is COPD?
COPD is a progressive (i.e. gets worse with time), chronic, inflammatory lung disease obstructing air-flow to the lungs, mainly caused by breathing pollutants.
To help understand what is going on with COPD, first see how the lungs work:
COPD damage reduces the natural elasticity of the alveoli (air sacs) and bronchial tubes. Elasticity is required to force out air/carbon dioxide for exhalation. As a consequence, unexpelled air is trapped in the lungs, which makes it difficult for the air sacs to deflate and bring in new air
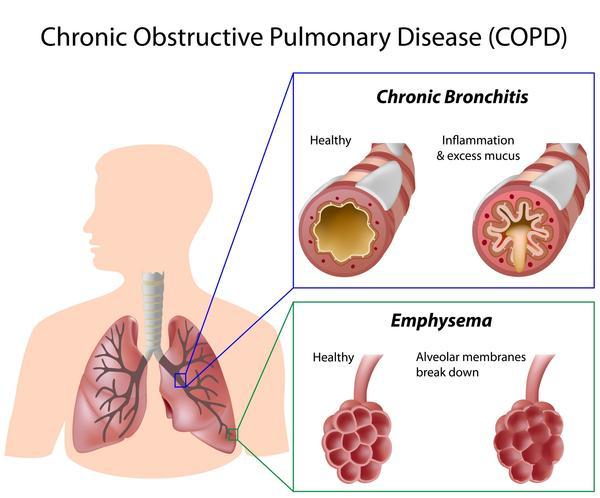
COPD describes several progressive lung diseases characterized by shortness of breath. Includes:
- CHRONIC bronchitis. The constant irritation/inflammation of the MUCUS MEMBRANE LINING (epithelium) of the bronchial airways (bronchi/bronchioles, which carry air to and from the alveoli of the lungs), causes it to swell and produce mucus, which narrows the airways, making it harder to breathe; a cough ensues to try and clear the mucus. FYI – Mucus membranes also line the sinuses, GI and urinary tracts
- Emphysema. Breakdown of the elastin of lung connective tissues weakens/damages the thin walls and fibers of the alveoli (air sacs) at the end of the smallest bronchial airways (bronchioles); the alveoli walls eventually break down, producing less, but larger air spaces instead of many small ones, and so reducing the surface area available for gas exchange;
- Non-reversible asthma
- Some forms of bronchietasis
COPD is the THIRD leading cause of death in the U.S. affecting ~30 million Americans. Of those, >50% are unaware they have it
COPD progression causes loss of lung function. Can increase risk for:
- Respiratory infections. E.g. flu, colds, pneumonia – making it even more difficult to breathe
- Lung cancer
- Pulmonary hypertension. High blood pressure in arteries delivering blood to lung
- Heart disease. Reason not well understood
COPD Diagnosis. A breathing test, called spirometry, measures the amount of air blown out of the lungs in how long. This simple test can detect COPD ahead of symptoms
COPD symptoms
Include:
Increased breathlessness – especially during activities
- Chronic / Ongoing cough (trying to clear produced sputum/mucus) – especially first thing in the morning
- Frequent repiratory infections
- Wheezing
- Blueness of lips or fingernail beds (cyanosis) – due to lower oxygen availability
- Chest tightness
Causes / Risk factors of COPD
Most COPD is caused by inhalation of pollutants. Including:
- Smoking (LEADING CAUSE IN U.S.) and second-hand smoke – ~90% of those with COPD have a history of smoking;
- Chemicals, fumes, dust in occupational environments – especially those who have had long term exposure
- In the developing world, breathing cooking fuel or poorly vented heating fumes
Being over 40 years old and male. Although most COPD deaths are women
Genetics. ~1% of those with COPD have a deficiency of liver-produced, lung-protective alpha-1 antitrypsin protein (AAt), which is the most commonly known genetic risk for emphysema – with the result that white blood cells (WBCs) are able to harm the lungs
>90% of bronchial infections are caused by a virus. Albert, RH (1 December 2010). “Diagnosis and treatment of acute bronchitis.”.American family physician(11): 1345-50. PubMed
How to treat COPD
Avoid irritants
- Stop smoking or breathing second-hand smoke
- Minimize occupational exposure to pollutants
Nebulize anti-infective “Medicine”
- Use a nebulizer to deliver an alternative antimicrobial medicine directly into the lungs.Choices of alternative antibiotics include ionic colloidal silver, grapefruit seed extract, hydrogen peroxide, iodine, magnesium chloride, glutathione and others;
Alternative medicines administered via a nebulizer
Ensure body contains sufficient magnesium and vitamin D
- The fastest way to increase magnesium presence in your body is to apply magnesium chloride oil (MCO) transdermally:
Transdermal Magnesium Chloride
- The best way to increase body’s vitamin D levels is to take a sunbath:
Taking a Sunbath for Vitamin D
Ensure anti-inflammatory components in your diet and Lifestyle
- Especially Omega-3
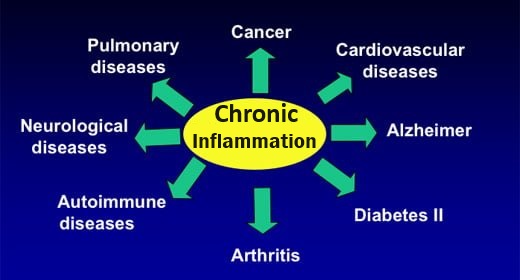
How to treat chroninc inflammation
Attend to health of mucus membranes
 Keep well hydrated – drink enough water; also breathing water vapor helps loosen mucus and makes breathing easier
Keep well hydrated – drink enough water; also breathing water vapor helps loosen mucus and makes breathing easier- Ensure sufficient dietary/supplementary antioxidants – to counter inflammation by reducing free radicals
- Herbs to soothe and lubricate mucus membranes – include slippery elm, marshmallow, licorice, mullein
- Consume zinc-rich foods – especially pumpkin seeds
- Nebulizing moistens mucus membranes
- Proteolytic enzymes – E.g. bromain, papain and serrapeptase all reduce inflammation, but serrapeptase especially helps break down excessive mucus