Atherosclerosis is a life-saving INFLAMMATORY RESPONSE to prevent you from bleeding to death!
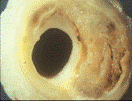
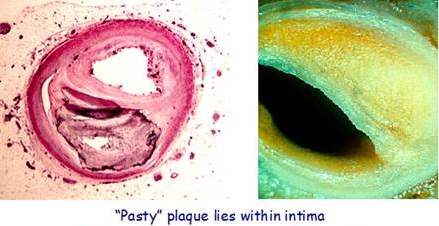
What is atherosclerosis? (Greek: athero=paste, sclerosis=hardening)
Atherosclerosis occurs as a result of the immune system’s INFLAMMATORY RESPONSE to an arterial blood vessel wall DAMAGE. Intended as a temporary fix, plaque (a paste mainly consisting of cholesterol and fat) is laid down to prevent bleeding out through a damaged arterial wall.
19th Century Inflamed Arteries
Based on his detailed autopsy studies and pathology investigations of those who had died of heart disease, late 19th century, German physiologist Rudolph Virchow proposed that the origin of heart disease was inflammation of the heart and the arteries. He found that their arteries looked as though they had been wounded inside, similar to an infected skin abrasion
Why be concerned about atherosclerosis?
Most cardiovascular disease (CVD) and peripheral artery disease (PAD) is a consequence of atherosclerosis. If the actual cause of arterial wall damage is not addressed, arterial plaques can grow in size, causing a narrowing (stenosis) of the arterial lumen. Not only does this increase blood pressure, but eventually it can block the smaller arteries – such as the coronary arteries providing blood to the heart (causing a heart attack), or a piece can break away from plaque, travel in the bloodstream and end up blocking / bursting the small arteries in the brain (causing strokes), or blocking peripheral arteries to the legs, feet or arms (causing pain and / or nerve / tissue damage), or setting the stage for several other undesirable possibilities:
- Coronary Heart Disease (CHD) – atherosclerosis narrows the coronary arteries
- Heart attack (myocardial infarction) – a blood clot develops from plaque, typically in one of the coronary arteries, causing a blockage, called a thrombosis), which blocks the oxygen supply to the heart
- Arrhythmia – irregular heartbeat
- Stroke – blockage of carotid artery supplying oxygenated blood to the brain
- Angina – chest pain
- Hypertension (high blood pressure)
- Thrombosis – clot formation attached to blood vessel wall in an artery or vein obstructing blood flow;
- Hemorrhagic burst (blood vessel rupture).
- Peripheral artery disease (PAD)
Atherosclerosis is sometimes accompanied by hardening of the artery lumen (arteriosclerosis), which eventually:
- Decreases circulation
- And reduces arterial elasticity
- Compromises the dilation of blood vessels when needed – such as during strenuous exercise.
Plaque accumulation (swelling) in an artery is always in the intima (between the endothelial lining and the smooth muscle wall)
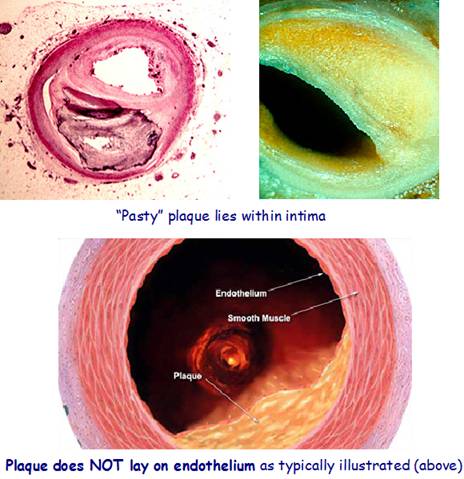
Atherosclerotic plaques characteristically occur in high pressure / turbulent areas in arterial blood vessels
In regions of branching and marked curvature at areas of geometric irregularity. i.e. where blood undergoes sudden changes in velocity and direction of flow.
It does not occur in veins carrying deoxygenated blood. i.e. under pressure 8 times lower than the arteries
Occurs In any medium / large artery supplying oxygenated blood under high pressure, but most frequently affects the following arteries:
- Aorta – Largest artery – supplies blood to all body parts. The aorta extends about 1 foot from the heart to the pelvis, however, plaque most commonly occurs in the abdominal aorta and if present there, it is probably in other arteries)
- Coronary arteries leading to coronary heart / artery disease (i.e. CHD or CAD). There are 2 main coronary arteries that branch off the aorta and supply blood to the heart muscle. Atherosclerosis/arteriosclerosis reduces their supply, leading to blood insufficiency (ischemia) to the heart;
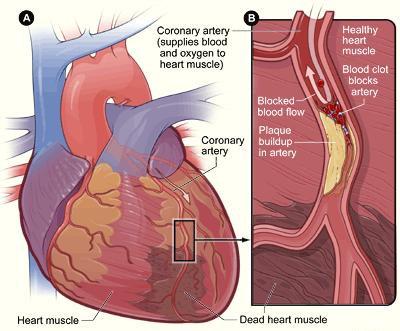
There’s that incorrect depiction of plaque placement again! 🙂
- Iliac / Femoral Arteries –atherosclerosis / arteriosclerosis causes a decrease in blood flow to the legs and feet that can injure nerves and other tissues.
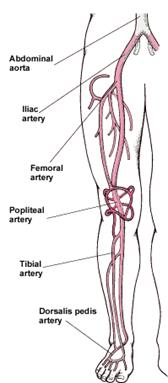
- Axillary / Brachial Arteries. Arm artery disease is a rare form of PAD, but the most common cause is atherosclerosis in the arm arteries, which can cut off circulation to the hand; symptoms include pain, weakness, fingers turning blue, and gangrene.
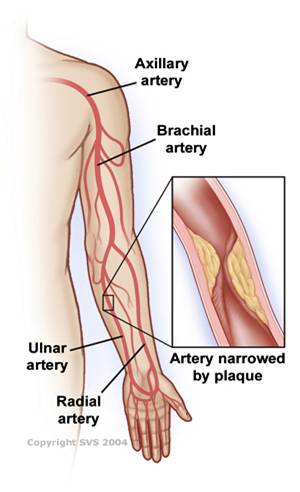
- Carotid and Vertebral Arteries. Atherosclerosis reduces the oxygen-rich blood supply to the brain. Carotid artery disease accounts for well over 95% of symptoms causing cerebrovascular disease. When the carotid arteries are obstructed, you are at an increased risk for a stroke.
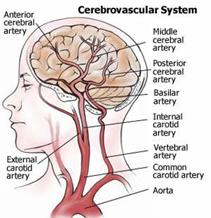
Why does atherosclerosis occur?
Contrary to popular opinion, although atherosclerosis / ischaemic CVD involves high blood cholesterol or triglycerides, it is NOT caused by them
CVD involving restricted blood flow due to atherosclerosis is a consequence of damage to an arterial wall weakened by a long-term, low-level deficiency of vitamin C
The body deals with a weakened arterial wall by initiating an inflammatory response to save your life – by placing a cholesterol-containing patch over the damage to prevent you bleeding out. This is meant to be a temporary measure, to buy you time to fix what is actually causing the damage and restrengthen the wall.
by adding dietary vitamin C for your body to be able to produce tissue-connective collagen.
Scurvy occurred in the 1700 and 1800’s on sailing ships due to lack of vitamin C. Thousands of lives were lost until limes were added to the ship’s food inventory on long overseas journies.
.
Several culprits can damage the arterial wall
(a) Mechanical / Hemodynamic stress
(b) Oxidant / Antioxidant Imbalance allowing damaging reactive oxygen species (ROS) and/or reactive nitrogen species (RNS) to go unchecked.
(c) Hyperglycemia (high blood sugar). A result of excessive intake of sugar / fructose / carbohydrate;
(d) Elevated homocysteine levels. A consequence of too much meat and/or dairy products;
(e) Overly acid-forming diet
Vitamin C deficiency is the primary cause of a weakened arterial wall
Vitamin C (together with the amino acids lysine and proline), maintain arterial structural integrity by their role in forming connective tissue components collagen and elastin. Arteries (and every other body tissue) constantly undergo decay, repair, and replacement. Tissue repair and replacement requires a binding protein called collagen, which the body produces using vitamin C (ascorbate). An insufficiency of ascorbate will cause artery walls to form lesions (wounds) as they fall into disrepair.
A chronic deficiency of vitamin C leads to chronic scurvy. Eventually the lesions would rupture and you would bleed to death through the arterial wall.
Atherosclerosis / CVD caused by weak walls due to chronic scurvy
Fix the wall / Prevent the injuries
Chronic inflammation of the endothelial cells (ECs) lining the arterial wall is caused by nutrient deficiencies and lifestyle choices. NOT by elevated cholesterol and calcium, whose deposits in the arteries are secondary to the primary causes.
“Cardiovascular DIY Fix” -♪”How can you mend a broken heart?”♪♫
Atherosclerosis process - How and why does atherosclerotic plaque build up in arteries?
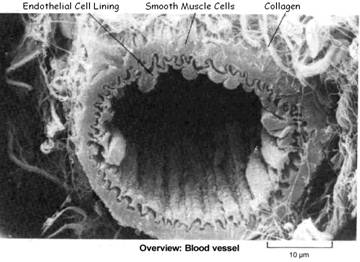
Endothelial cells (ECs) lining the inside of the artery function as a barrier. ECs prevent toxic substances in the blood from entering the elastic smooth muscle in the middle of the vessel wall.
In response to various injurious mechanisms to a weakened endothelial artery lining the arterial wall ECs initiate life-saving action to “beef up” the damaged wall by depositing an artery-thickening layer of plaque.
- Chronic injury by various injurious mechanisms to ECs in a weakened artery lining irritates and inflames the endothelium causing the ECs to initiate a “life-saving” inflammatory immune response for the purpose of “beefing up” the damaged wall. This involves a complicated series of steps, including T-cell activation, foam-cell formation, smooth muscle migration, and blood platelet adherence and aggregation for the purpose of depositing an artery-thickening plaque over the damaged area to prevent a person from bleeding out through a ruptured blood vessel (usually under high pressure). This process is called atherosclerosis.
(1) The ACUTE PHASE inflammatory response is a necessary and appropriate response to injury or infection
Without inflammation infections would go unchecked and wounds would never heal. The damaged site becomes red, swollen and warm as healing mechanisms are initiated. The acute phase response occurs within minutes to hours, but if the infection or injury continues and/or the problem is not resolved within a few days, it becomes a chronic inflammatory response.
Acute phase protein (APP) molecules (cytokines and acute phase reactants) orchestrate the responsive action
- Released in response to alarm-signaling cytokines (particularly IL-6) – by most cells (in particular in the arteries, by various immune system cells, E.g. T-cells, macrophages, platelets, and ECs) during infection or injury;
- Acute Phase Reactants (APRs, a type of APP) are produced (mostly in the liver) and released into the plasma –modulate blood clotting, vessel dilation/ contraction, fibrosis (repair fiber/scarring), cell proliferation, immune cell action, cholesterol deposit/removal, and more.
Acute Inflammation Response
- Vessels dilate for 15 minutes to several hours and become more permeable. Enabling WBCs and fluids to leave the vessels (manifests as swelling);
- Phagocytic WBCs adhere to vessel wall. Cytokines increase number of EC adhesion molecules, which then adhere phagocytic WBCs (usually neutrophils) to the vessel wall, which engulf and destroy microbes and debris particles. (In viral infection, lymphocytes rather than neutrophils usually predominate. In certain parasitic infections, eosinophils predominate);
- Injurious agents are destroyed or walled off and debris is cleared. By activated specialized blood and connective tissue cells, so that tissue repair can take place;
- Blood clot is formed. To prevent blood loss and provide a barrier to microorganisms;
- Fibrous connective tissue is brought in to repair the damage;
- When healing is complete the blood clot is removed.
(2) CHRONIC inflammatory response leads to endothelial dysfunction and eventually the development of atherosclerotic plaque
Inappropriate, prolonged inflammatory response to ongoing endothelial injury leads to:
- Endothelial dysfunction as a consequence of sustained vessel constriction / high blood pressure (mainly as a consequence of insufficient available, endothelium-relaxing nitric oxide)
- Further increases in coagulation, vessel adhesion molecules, and immune system white blood cell activity.
- The process culminates in the development of atherosclerotic plaque.
Chronic inflammation in the arterial endothelium involves:
- Vessel constriction. Due to failure of endothelium-dependent relaxation mechanism;
- Macrophages and Lymphocytes. Accumulation of immune system macrophages (engulf and destroy bacteria / debris/cholesterol) and lymphocytes (T-cells, B-cells, NK cells);
- Tissue Damage. Generation of damaging ROS in ECs, smooth muscle cells (SMCs) and adventitia, responsible for tissue destruction, as seen in CVD (and auto immune and neurodegenerative disease);
- Life-saving Atherosclerotic Plaque. Chronic endothelial injury requires a more substantial, artery-thickening, “repair patch”as a life-saving measure to prevent arterial rupture (artery is under high pressure), consisting of oxidized cholesterol, fat, smooth muscle cells, macrophages, T-cells, fibrous tissue and calcium deposits.

This stronger repair process involves:
- Vascular smooth muscle cell proliferation
- Development of fibrosis – excess fibrous connective tissue, mainly collagen and elastin.
- Accumulation of cholesterol – which becomes oxidized and develops into foam cells and fatty streaks (via immune system monocytes/macrophages).
(3) Eventually the artery is partially or fully occluded
- By the physical obstruction of atherosclerotic plaque itself
- Or more often by blood clots (thrombi) formed by plaque rupture, which results in reduction of blood flow (ischemia)
- Or by a piece of plaque breaking off and traveling to and blocking smaller arteries, such as the carotid artery
Possibly resulting in:
- Damage to heart muscle (by blocking a coronary artery) →→→HEART ATTACK
- Damage to brain (by blocking a carotid artery) →→→ STROKE / CAROTID ARTERY DISEASE (>95% of cerebrovascular disease)
- Damage to nerves and tissues in legs and feet (by blocking an iliac artery) →→→ PERIPHERAL ARTERY DISEASE (PAD)